what is a common analgesic administered to control a moderate level of pain?
Pain is one of the near common concerns of patients presenting to the ED. Achieving excellent analgesia while minimizing side effects is an important and nuanced skill to develop. The goal of emergency hurting management is not to completely eradicate pain merely rather, reduce pain to an acceptable level allowing for prophylactic discharge/return to daily activities, or to bridge until inpatient intendance can be arranged 1,2 .
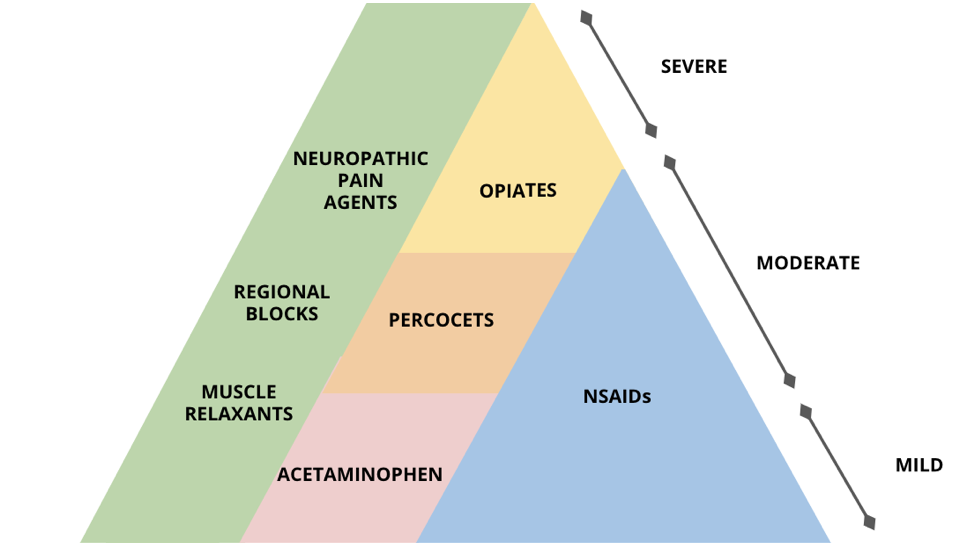
There are a number of principles of pain management to go along in mind when choosing an analgesic agent. The WHO Analgesic Ladder has been a ofttimes cited reference for decades and has five main themes to guide your choices iii :
- Oral administration is preferred whenever possible
- Analgesics should be given regularly enough to maintain pain control
- Agents should be chosen based on reported pain intensity
- Dosing of agents should be adapted to the patient
- Patients should be given clear instructions on how/when to take their medications
The type of pain that a patient is experiencing and their medical history (e.g. medical conditions, drug allergies, current medications, etc.) will influence your analgesic choice equally well but a basic understanding of what your options are and when to use them is a adept starting point. This post will give you an introduction to the types of analgesics you have access to in the emergency section and when to use them.
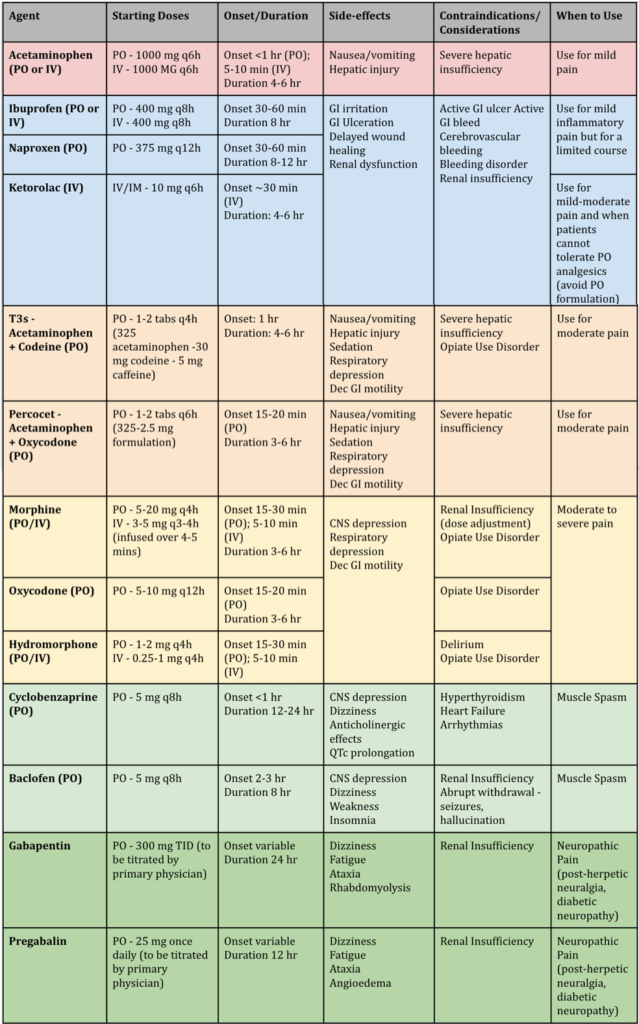
Acetaminophen (Mild Pain)
Acetaminophen (Tylenol) is oft a starting time line agent in the ED for mild pain. This is because of the efficacy for balmy pain as well equally the minimal side effects that come with information technology. Because tylenol is metabolized past the liver, astringent hepatic insufficiency is a contraindication but otherwise it is quite a universal analgesic 1,2 .
NSAIDs (Balmy-Moderate Hurting)
NSAIDs are an excellent choice for mild to moderate pain secondary to inflammation. This form of drugs is diverse and its uses can vary from MSK pain to renal colic. NSAIDs are often used as a offset line agent either alone or in combination with acetaminophen. Despite their efficacy, NSAIDs have been associated with gastric bleeding, ulcers, platelet function inhibition, and nephrotoxicity. These adverse effects necessitate that these agents are used for a curt course and are avoided in patients with renal disease. Mutual NSAIDs used in the emergency section include Ibuprofen (Advil), Naproxen (Aleve), and Ketorolac (Toradol) one,2,4 . Each drug has characteristics that define the best context to use it in:
- Ibuprofen – Oral drug – best GI side effect profile
- Naproxen – Oral drug – best cardiovascular side effect contour
- Ketorolac – Iv/IM drug – all-time for patients who cannot tolerate PO analgesia (typically used for moderate pain) ***Notation: A PO formulation exists but should be avoided due to higher side issue profile despite similar analgesic outcome 4
Opiates (Moderate-Astringent Hurting)
Opiates are effective analgesic agents in the context of moderate to severe acute pain that cannot be fairly controlled with a non-opiate. However, this efficacy is coupled with a number of harmful side effects including: respiratory depression, sedation, tolerance, hyperalgesia, and opioid use disorder. For any outpatient script, recollect that opioids are extremely constipating and so e'er write a laxative script aslope the opioid. Great care must exist taken to prescribe these drugs responsibly and under the right circumstances after appropriately educating patients about the risks and the analgesic alternatives.
The most commonly used opiates include morphine, oxycodone, and hydromorphone. Combination drugs similar T3s and Percocets are often used to target moderate pain merely importantly have the aforementioned addictive backdrop of other opiates. At equianalgesic doses, the efficacy of different opiates is the same (allowing for variance in metabolism). Often, the type of opiate used is influenced by the practitioners familiarity with dosages. Regardless when titrating opiates, "start low, become slow" is a practiced arroyo to prevent overdosing. For the elderly, it is essential to use circumspection as opioids tin build up leading to delayed narcotic overdose 1,two,5–7 .
- Combination drugs:
- T3s (acetaminophen + codeine)
- Percocet (acetaminophen + oxycodone) for moderate pain
- Morphine:
- Baseline by which other opiates are measured (ME = morphine equivalents)
- Annotation: metabolites hard to excrete in renal failure
- Oxycodone (i.5 ME)
- Hydromorphone (5 ME)
- Neuro-excitatory metabolites difficult to excrete so increased adventure of delirium
The addictive nature of opiates is something to go along in the forefront of your mind when choosing what is best for your patient. Important questions to ask yourself include: Is my patient opioid naive? Is there a history of substance abuse? What is the take chances of prescribing short-course PRN opioids on discharge for my patient? The Opioid Hazard Tool (ORT) is a quick tool to take risk factors into consideration when making this difficult decision. In patients with elevated risk, y'all may choose agents with less addictive potential like NSAIDs, non-opioid analgesics or a cursory opioid grade with counseling. Call back that even a brusk term prescription carries with information technology real risks of creating opioid dependency. In high risk patients, consider dispensing or prescribing a naloxone kit. Propose patients to safely dispose of their opioids and to lock them upward if in that location are dependents in the house who could inadvertently overdose through misadventure or error 7 .
Muscle Relaxants (Muscle Spasm)
Muscle relaxants are a class of drugs that are used to treat hurting secondary to musculus spasm. Many musculus relaxants come with side effects including drowsiness and dizziness. This can proceed patients from staying agile and getting dorsum to their baseline function (which are the goals of managing spasm/hurting). Keeping in mind the common side effects of muscle relaxant use, information technology is recommended to utilize them in low quantities for short durations and to advise patients to avoid combining these with opioids, alcohol or benzodiazepines. Common musculus relaxants used in the emergency department include baclofen (Lioresal) and cyclobenzaprine (Flexeril) viii,9 .
Neuropathic Pain Medications (Nerve Pain)
Nerve pain is a common concern in the ED simply it is often hard to treat in this setting. The claiming stems from the wearisome onset of these medications (days to weeks) and necessity of titration to effect. The about common medications used to treat neuropathic pain are calcium channel blocker anticonvulsants including gabapentin and pregabalin. Both of these drugs have an unattractive side effect contour, despite their efficacy in cases of postherpetic neuralgia and diabetic neuropathy. Mutual adverse effects include dizziness, fatigue, clutter, and rhabdomyolysis. They are excreted renally and should exist avoided in those with renal insufficiency. When prescribing these, start at low doses earlier titrating up and advise patients to monitor for side effects. These should also be used in caution with patients already taking narcotics as they also have abuse potential 10 .
Other Options
Regional Blocks
Nerve blocks are useful when pain is well localized in an area or nerve distribution (due east.thou. single digit, sciatica, dental). Regional blocks take the do good of prolonged elapsing of pain relief but come with the cost of time needed to perform the procedure as well as risks associated with needle insertion. This is often a technique performed past more experienced or specially-trained practitioners in the department. Mutual agents used include lidocaine (shorter acting) and bupivacaine (longer-acting). Either amanuensis tin can be combined with epinephrine to cause vasoconstriction, delaying anesthetic distribution and prolonging duration of effect. Although this is not a universally common procedure, interest has been gaining in this method of pain direction in the ED eleven .
Adjuncts/Non-Pharmacologic Treatments
As adjuncts to medication don't forget that the mind plays an of import part in pain. Endeavour and ensure they have a comfortable position to sit in (where space allows). Administer ice or heat and use splints for MSK injuries. Utilize lark (smart phones, ipads) where possible. For young children, carbohydrate-based solutions can be used to mitigate painful procedures. Studies have shown that telling patients that their pain will exist reduced tin can help magnify the impact of handling 11,12 .
There are a number of offshoot therapies that can exist used in conjunction with the above mentioned therapies. Water ice and estrus therapy is a common recommendation for MSK pain. Sprains and strains take been shown to respond well to topical NSAIDs like diclofenac (Voltaren). Part of your disposition program should e'er involve a program to return to action if this is limited by a patient's pain. Often, a multimodal arroyo to pain direction is the nearly efficacious i 11 .
Takeaways
- The goal of pain-direction in the ED is not nil pain, but rather reaching an acceptable level for function.
- When choosing route of delivery, oral is ofttimes preferred unless the patient cannot tolerate PO meds.
- Consider a combination of non-opiates. Starting with 1000 mg Acetaminophen and 400 mg of Ibuprofen is an ED go-to for balmy-moderate hurting.
- Opiates should simply be used if non-opiate agents are insufficient to treat the severity of pain that the patient endorses. When using opiates, start low and get deadening!
- Treat pain before ordering your workup! Do non leave your patient suffering until you get results back.
Final Thoughts
You will inevitably manage pain during every ED shift but luckily you lot have a diverse arsenal of agents at your disposal. As we continue to learn about how these agents compare, practice volition shift and information technology is important to reassess why you are choosing one drug over another. When managing your patient'south pain make certain you residuum efficacy with the risks associated with each agent. Always adopt a patient-centered approach and counsel extensively on the risks and side furnishings of each agent.
This mail service was edited by Megan Chu and Julia Heighton, and posted by Megan Chu.
-
ane.
Optimizing the Treatment of Acute Pain in the Emergency Department. Annals of Emergency Medicine. September 2017:446-448. doi:10.1016/j.annemergmed.2017.06.043
-
two.
Cisewski DH, Motov SM. Essential pharmacologic options for acute hurting management in the emergency setting. Turkish Periodical of Emergency Medicine. Jan 2019:ane-eleven. doi:10.1016/j.tjem.2018.eleven.003
-
three.
Forbes K. Hurting in Patients with Cancer: The World Health Organization Analgesic Ladder and Across. Clinical Oncology. August 2011:379-380. doi:10.1016/j.clon.2011.04.016
-
iv.
Nissen SE, Yeomans ND, Solomon DH, et al. Cardiovascular Safety of Celecoxib, Naproxen, or Ibuprofen for Arthritis. N Engl J Med. December 2016:2519-2529. doi:10.1056/nejmoa1611593
-
5.
National Pain Center MGD. Canadian Guideline for Safe and Effective Utilise of Opioids for Chronic Not-Cancer Hurting. Canadian Guideline for Safe and Constructive Employ of Opioids for Chronic Non-Cancer Pain. http://nationalpaincentre.mcmaster.ca/opioid/cgop_b_app_b08.html. Accessed March 26, 2020.
-
6.
Banerjee Chiliad, Bhaumik D, Ghosh A. A comparative study of oral tramadol and ibuprofen in postoperative hurting in operations of lower abdomen. J Indian Med Assoc. 2011;109(9):619-622, 626. https://world wide web.ncbi.nlm.nih.gov/pubmed/22480093.
-
vii.
Barnett ML, Olenski AR, Jena AB. Opioid-Prescribing Patterns of Emergency Physicians and Run a risk of Long-Term Use. N Engl J Med. February 2017:663-673. doi:10.1056/nejmsa1610524
-
eight.
Witenko C, Moorman-Li R, Motycka C, et al. Considerations for the appropriate use of skeletal muscle relaxants for the management of astute low dorsum pain. P T. 2014;39(half dozen):427-435. https://www.ncbi.nlm.nih.gov/pubmed/25050056.
-
ten.
Freynhagen R, Busche P, Konrad C, Balkenohl Grand. [Effectiveness and fourth dimension to onset of pregabalin in patients with neuropathic pain]. Schmerz. 2006;20(four):285-288, 290-292. doi:x.1007/s00482-005-0449-0
-
xi.
Derry South, Wiffen P, Kalso E, et al. Topical analgesics for acute and chronic pain in adults – an overview of Cochrane Reviews. Cochrane Database Syst Rev. 2017;5:CD008609. doi:ten.1002/14651858.CD008609.pub2
-
12.
Gates Thou, Hartling L, Shulhan-Kilroy J, et al. Digital Technology Lark for Acute Hurting in Children: A Meta-analysis. Pediatrics. January 2020:e20191139. doi:10.1542/peds.2019-1139
Reviewing with the Staff
The ED is a painful place for patients, between long waits, non-ergnomic chairs and crowding, it can be hard to go comfortable. Call back about hurting every bit one of those initial vital signs and do what you can to condolement and ease patients. Call up, nigh of usa got into this to endeavour and help people, to be healers, and providing compassion and condolement are essential parts of that service. My starting time step is to always consider what I can do in addition to medications, can I provide solace, assistance a patient reposition, is there some mode to distract them?
For virtually hurting, starting with a combination of acetaminophen and a nsaid (assuming no contraindications) is a prophylactic place to start and really demonstrates like efficacy to opioids for MSK complaints. For patients who need to be NPO, consider if an NSAID (like ketorlac) can be used; for renal colic it has been shown to be superior to opioids.
The opioid crisis has really changed the lens through which we view pain. Whereas initially opioids were touted as a panacea, we are at present aware of their addictive potential and that they cause hyperalgesia and worse decease. They are directly responsible for truncated lifespans and a generation of lost souls. It led to an early on modify in my do to exist more cognizant of the real chance of outpatient pain medications. Studies have shown that if individuals leave the ED with a narcotic script, they have an increased chance of overdose and opioid dependence. This became at odds with my desire of healing - if we tin't 'cure' pain and so how do we move forward? This reminds the states how important the conversation is with patients. Now when because outpatient analgesia, I screen using the ORT, I walk patients through the pyramid and talk well-nigh the risks and benefits of dissimilar classes, I assess how their pain has been controlled in the ED and consider how severe their ailment is and consider potential interactions with home medications. Hurting control requires an individualized approach.

Alim Nagji
Alim Nagji is an ER staff at Joseph Brant (JBH) & St. Joseph Healthcare Hamilton. He is the Director of Emergency Medicine Clerkship for McMaster University and the Director of Simulation Learning and Clinical Teaching Unit for JBH. He has interests in medical didactics, simulation and global health. Send him your favourite meme on twitter @alimnagji
(Visited 13,106 times, 3 visits today)
Source: https://canadiem.org/approach-to-pain-management-in-the-ed/

0 Response to "what is a common analgesic administered to control a moderate level of pain?"
Post a Comment